The word ‘viable’ — which carries the specific medical meaning that your baby could now survive outside the womb with intensive NICU support — applies. That is a sentence that means something real and documented: survival rates for babies born at 24 weeks in modern US medical facilities are approximately 42–70% with intensive neonatal care, according to data from ACOG and national hospital databases. One week ago at Week 23, the number was lower. Next week at Week 25, it will be higher. Between now and Week 26, survival probability increases 2–4% with every single day the baby remains in the womb.
At 24 weeks pregnant, your baby is the size of an ear of corn — approximately 30cm (nearly 12 inches) from head to toe and weighing around 600 grams, which is just over a pound and a third. The face is fully formed and would be recognizable as the face you will see at birth. And two of the most remarkable developmental milestones of the entire second trimester are happening right now: the eyelids are beginning to prepare to open — the cornea is developing, the retina’s layers are forming, and by Week 26–28, the eyes will open for the first time — and the taste buds are completely developed, connected and functional, meaning your baby is tasting the flavors of what you eat as they pass through the amniotic fluid.
Week 24 is also the week that gestational diabetes screening is officially scheduled — the glucose challenge test (GCT) that most OBs order between Weeks 24–28. At Babyslover, here is the complete Week 24 guide: viability explained fully and without alarming oversimplification, the taste and eye development milestones, the GD screening walkthrough so you know exactly what to expect, and everything your body is doing as you move one week closer to the third trimester. Coming from last week? Our 23 weeks pregnant guide covered voice recognition and the inner ear milestone in depth.

| 📋 Quick Summary — Week 24 of Pregnancy | |
| Week | Week 24 of 40 — Second Trimester, Week 12 (Final weeks of second trimester beginning) |
| Baby Size | 🌽 Ear of Corn — ~30cm head-to-heel (11.8 inches) |
| Baby Weight | ~600 grams (1.3 lbs) — gaining ~100g per week |
| ✅ KEY MILESTONE | ✅ VIABILITY WEEK REACHED — baby can now survive outside the womb with NICU support (42–70% survival at 24 weeks). Every day from here adds 2–4% to the odds. |
| Baby Milestones | 👁️ Eyelids preparing to open (cornea developing, retina maturing — will open Week 26-28!) • 👅 Taste buds FULLY FORMED — baby tasting amniotic fluid flavors now! • 🫁 Surfactant increasing in lungs • Skin thickening, fat deposits building • Brain continuing fastest growth • Meconium (first stool) forming in intestines |
| Medical This Week | 🩺 GESTATIONAL DIABETES SCREENING — glucose challenge test (GCT) happens now! 24–28 weeks standard window per ADA/ACOG guidelines. |
| Symptoms | Round ligament pain, linea nigra darkening, iron deficiency anemia (fatigue, breathlessness), Braxton Hicks increasing, sleep disruption, heartburn worsening, back pain, pregnancy brain continuing, stretch marks may appear, swollen feet/ankles |
| Act Now | Schedule GD screening if not yet booked. Continue talking/singing/reading to baby daily. Begin hospital tour booking. Start or continue hospital bag list. |
Contents
- 1 ✅ What Does Viability at 24 Weeks Actually Mean?
- 2 🌱 Baby Development at 24 Weeks Pregnant
- 3 🩺 Gestational Diabetes Screening — Your Complete GCT Guide
- 4 What’s Happening in Your Body at 24 Weeks Pregnant
- 5 Nutrition at 24 Weeks — The Iron-Plus-C Strategy
- 6 For Your Partner — Week 24 Actions
- 7 When to Call Your Doctor at 24 Weeks Pregnant
- 8 Your Week 24 Pregnancy Checklist
- 9 Frequently Asked Questions — 24 Weeks Pregnant
- 10 💗 The Emotional Reality of Week 24 — You Made It Here
- 11 👶 What’s Next — 25 Weeks Pregnant Preview
- 12 Week 24: The Corn That Can Taste Your Cooking
✅ What Does Viability at 24 Weeks Actually Mean?
‘Viability’ is one of the most emotionally loaded words in pregnancy. It is worth understanding what it means precisely — not more and not less than what the data actually shows.
Viability means: survival outside the womb is medically possible with intensive NICU support. It does not mean survival is likely at every facility, guaranteed in every situation, or without significant risk of complications. The survival rates at 24 weeks range considerably depending on the quality of the neonatal intensive care unit, the baby’s individual development, birth weight, sex (girls statistically have somewhat better outcomes at extreme prematurity), and other clinical factors.
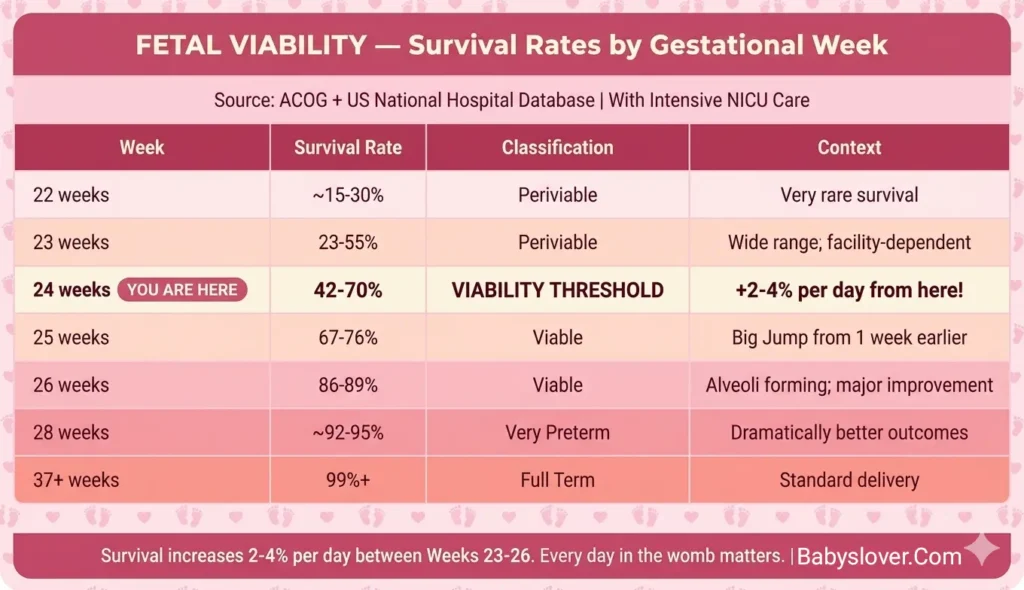
| Week | Survival Rate | Classification | Context |
| 22 weeks | ~15–30% | Periviable | Very rare survival; significant ethical debate |
| 23 weeks | 23–55% | Periviable | Broad range; facility-dependent; 23 wks exactly is the threshold of possible |
| 24 weeks ← YOU ARE HERE ✅ | 42–70% | ✅ VIABILITY THRESHOLD | Survival now possible at most advanced NICUs; +2-4%/day |
| 25 weeks | 67–76% | Viable | Significant improvement from one week earlier |
| 26 weeks | 86–89% | Viable | Lungs developing air sacs; major jump in outcomes |
| 28 weeks | ~92–95% | Very Preterm | “Very preterm” — major developmental head start vs 24-26 wks |
| 37+ weeks | 99%+ | Full Term | Term delivery; standard neonatal outcomes |
The critical fact embedded in this table: between Weeks 23 and 26, survival probability increases by approximately 2–4 percentage points per day. Not per week — per day. Each 24 hours the baby remains in the womb in this window adds meaningfully to the odds. This is why every effort to prevent preterm labor in this window — recognizing the warning signs early, reporting symptoms without delay, following rest and activity recommendations — matters as much as it does.
💡 The best NICU in the world is the womb. Every week from here through Week 40 is development that doesn’t have to be done under lights, on a ventilator, with tubes. Your body is doing something extraordinary — and the data shows what each week is worth. 💗
🌱 Baby Development at 24 Weeks Pregnant
At 24 weeks pregnant, your baby is approximately 30cm (11.8 inches) long from head to heel — the size of an ear of corn — and weighs about 600 grams (1.3 pounds). The face is now fully formed in all its proportions: the nose is defined, the lips are distinct, cheeks are rounding slightly as fat deposits begin to fill them out, and the ears — which have been functional for several weeks — sit in their final position. A photograph of a 24-week baby in utero would be recognizable as the face you will see at birth.
| 🌱 Baby Development at 24 Weeks | |
| Baby Size | 🌽 Ear of Corn — ~30cm head-to-heel (11.8 inches) |
| Weight | ~600 grams (1.3 lbs) — gaining ~100g per week! |
| KEY MILESTONE | ✅ VIABILITY THRESHOLD REACHED — survival with NICU support now possible. Survival rates: 42–70% at 24 weeks, improving 2–4% per day. |
What Is Developing at Week 24
- 👁️ Eyelids beginning to prepare to open — the eye is taking shape: Since early in the second trimester, the eyelids have been fused shut — sealed to protect the developing cornea and retina from the amniotic fluid environment. At Week 24, the cornea is developing its full structure and the retina is maturing its distinct cellular layers: the photoreceptors (rods and cones), the ganglion cells, and the layers that connect them. The eyelids will unseal and open for the first time around Week 26–28. Once open, the baby will be able to detect light and darkness — and the flashlight trick (placing a flashlight against the belly) will cause the baby to turn toward or away from the light source. The retina will not be fully mature at 24 weeks — complete visual development continues through the first year after birth — but the structural groundwork is being laid this week.
- 👅 Taste buds fully formed — your baby is tasting what you eat: The taste buds — approximately 10,000 of them across the tongue, palate, and throat — are structurally fully developed at Week 24 and are connected to the nervous system in a functional way. The baby swallows approximately 400–500ml of amniotic fluid daily (a figure that has been increasing since Week 16), and the flavor compounds from the foods you eat — garlic, vanilla, citrus, spices — cross the placenta and enter the amniotic fluid. The baby detects these flavors with the now-complete taste system. Research consistently demonstrates that newborns show preferences for flavors experienced in the womb: babies whose mothers regularly ate garlic during pregnancy show less negative response to garlic flavor postnatally. The prenatal taste experiences happening from this week onward are believed to form the foundation of early flavor preferences. Eating a varied diet of vegetables, spices, and diverse foods from here through the end of pregnancy introduces the baby to the flavor landscape they will encounter during weaning.
- 🫁 Surfactant increasing — the lungs are preparing: As covered in the Week 22 guide, type II pneumocytes began producing surfactant — the lung-coating substance that prevents air sacs from collapsing between breaths. At Week 24, surfactant production is measurably increasing. The lungs are not yet capable of sustained independent breathing, but the critical infrastructure is developing: the pulmonary capillary network (blood vessels surrounding the alveoli for gas exchange) continues growing, the terminal sac stage of lung development is underway, and the diaphragm is practicing its rhythmic contractions. Babies born at 24 weeks require respiratory support — ventilators and exogenous surfactant given as medication — but the biological machinery for breathing is actively under construction.
- 🧠 Brain and nervous system: rapid progress: The cerebral cortex is continuing its rapid folding — gyri and sulci (ridges and grooves) are becoming more defined, dramatically increasing the brain’s surface area and neural capacity. The cerebellum (balance and motor coordination) is growing quickly. Myelination — the process of coating nerve fibers with the insulating sheath that makes neural signals fast and efficient — is accelerating in the brainstem and spinal cord, which will govern the automatic functions the baby needs first at birth: breathing regulation, heart rate, swallowing, and basic reflexes.
- 💩 Meconium forming in the intestines: Meconium — the first stool, which is dark greenish-black, thick, and odorless — is beginning to accumulate in the intestines from swallowed amniotic fluid, shed cells, mucus, and early digestive secretions. This is the stool that healthy newborns typically pass in the first 24–48 hours after birth. Its presence in the intestines from this week onward is a normal sign of a functioning digestive system. If meconium is passed into the amniotic fluid before birth (meconium aspiration), it can be a concern at delivery — but meconium in the intestines itself is a normal and expected development from Week 24 onward.
- 🌡️ Fat deposits building under the skin: The skin, still thinner than a full-term baby’s, continues filling in as subcutaneous fat builds beneath the surface. The fine hair (lanugo) covering much of the body is still present — it will shed in the third trimester as fat takes over the insulation function. The vernix caseosa (waxy white coating) continues to thicken. Week by week, the ‘wrinkly’ appearance of an extremely premature baby gives way to the rounder, smoother look of a nearer-term newborn.
💡 Fun fact: Your baby can now taste garlic. If you eat garlic bread this week, the flavor compounds will cross the placenta, enter the amniotic fluid, and reach your baby’s fully formed taste buds. Research shows babies exposed to garlic, carrots, and vanilla prenatally show more positive responses to those flavors after birth. Eat diversely — you’re stocking the flavor library! 👅
🩺 Gestational Diabetes Screening — Your Complete GCT Guide
The glucose challenge test (GCT) — gestational diabetes (GD) screening — is one of the most discussed and most misunderstood prenatal tests. Most women in the US are offered it between Weeks 24–28, and Week 24 is when many OBs schedule it. Understanding exactly what it involves, what the numbers mean, and what happens if you need further testing takes almost all of the anxiety out of it.
Why Does Screening Happen at Week 24?
Gestational diabetes — a form of diabetes that develops during pregnancy due to hormonal interference with insulin function — most commonly develops in the second and third trimesters as the placenta produces increasing amounts of hormones (particularly human placental lactogen) that promote insulin resistance. The peak of this hormonal effect aligns with Weeks 24–28, which is why screening is timed here. Earlier in pregnancy, the hormonal load is lower and false negatives are more common; later, GD that developed earlier would already be causing complications. The American Diabetes Association and ACOG both recommend universal screening at 24–28 weeks for all pregnant women not already diagnosed with pre-existing diabetes.
The Two-Step Approach (Most Common in the US)
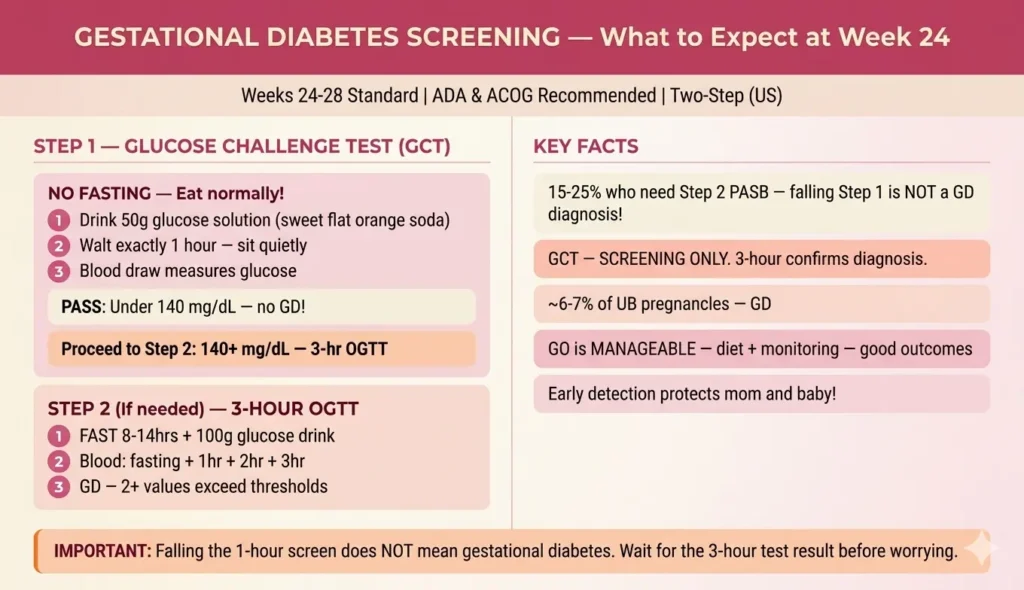
Step 1 — Glucose Challenge Test (GCT):
- No fasting required — you can eat normally before this test
- At the lab or OB office: you drink a 50-gram glucose solution (typically a sweet orange or cola-flavored drink — like a very sweet flat soda)
- You wait exactly one hour, sitting quietly (walking or activity affects results)
- A single blood draw measures your blood glucose level
- PASS (most women): Blood glucose below 140 mg/dL — no gestational diabetes screening needed, done!
- Proceed to Step 2: Blood glucose 140 mg/dL or higher → the 3-hour OGTT is scheduled
Step 2 — 3-Hour OGTT (if needed after Step 1):
- Fasting required: nothing to eat or drink except water for 8–14 hours before
- 100-gram glucose solution is consumed
- Blood drawn at fasting baseline, then 1 hour, 2 hours, and 3 hours after drinking
- GD is diagnosed if 2 or more values exceed thresholds: Fasting ≥95 mg/dL, 1hr ≥180 mg/dL, 2hr ≥155 mg/dL, 3hr ≥140 mg/dL
🚨 IMPORTANT: Failing (or ‘not passing’) the 1-hour GCT does NOT mean you have gestational diabetes. The GCT is a SCREENING test — it casts a wide net to identify who needs the more accurate 3-hour test. Approximately 15–25% of women who screen positive on the 1-hour pass the 3-hour with no GD diagnosis. One number on one blood test does not equal a diagnosis. Wait for the full picture before worrying.
If GD is diagnosed after the 3-hour OGTT: the condition is very manageable. Most women with GD control blood sugar effectively through dietary modification and exercise monitoring alone. A smaller number require insulin or oral medication. GD diagnosed and managed appropriately carries good outcomes for both mother and baby. The key is the diagnosis and management — undetected, unmanaged GD has real risks (large baby, difficult delivery, newborn blood sugar issues). This is exactly why the screening exists.
What’s Happening in Your Body at 24 Weeks Pregnant

😴 Iron Deficiency Anemia — The Week 24 Peak
Blood volume in pregnancy increases by approximately 40–50% from pre-pregnancy levels — the largest increase happens between Weeks 20–28, peaking around the same time as your GD screening. This dilutional effect — plasma volume expanding faster than red blood cell production can keep up — means many women experience the worst of their pregnancy anemia in Weeks 24–28, even if their iron intake is adequate. Symptoms: fatigue that seems disproportionate to activity level, breathlessness when climbing stairs or walking, heart palpitations, headaches, pallor, and difficulty concentrating. Your OB will check hemoglobin levels at this prenatal visit alongside the GCT. If iron levels are low, supplemental iron (beyond the prenatal vitamin) is typically recommended. Vitamin C alongside iron supplements and iron-rich foods (beef, spinach, lentils, fortified cereals) significantly improves absorption. Discuss specific supplementation levels with your OB — too little iron is common; too much can cause constipation.
〰️ Round Ligament Pain — Sharp Twinges on Side Movement
The round ligaments — two cord-like structures that run from the uterus to the groin — are being stretched rapidly as the uterus grows. The characteristic pain: a sharp, sudden twinge on one or both sides of the lower abdomen, triggered by fast movement — rolling over in bed, standing quickly, laughing, coughing, or sneezing. It typically lasts only seconds. Round ligament pain is entirely normal and not dangerous, but it can be alarming when first experienced. Management: slow, deliberate movements when changing position; warming the area with a heating pad (low setting); support belt or belly band; and knowing that the sensation, while sharp, is not a sign of anything wrong. Distinguish from cramping: round ligament pain is brief, sharp, clearly triggered by movement, and stops quickly. Cramping that is rhythmic, persistent, or comes with discharge or pressure requires OB contact.
🌑 Linea Nigra — The Dark Line Appears
Many women notice a dark vertical line running from the navel down to the pubic area — sometimes from the navel up to the rib cage — appearing or darkening around Week 20–24. This is the linea nigra (Latin: ‘black line’), caused by the same pregnancy hormones (especially melanocyte-stimulating hormone and estrogen) that darken the areolas, cause melasma (pregnancy mask), and make sun exposure more likely to cause hyperpigmentation. The linea nigra is completely benign, requires no treatment, and typically fades within several months after delivery as hormone levels normalize. Sun protection (sunscreen on exposed skin) reduces its intensity but doesn’t eliminate it during pregnancy.
🌙 Sleep — Getting Harder, Solutions That Work
Sleep disruption accelerates from Week 24 onward as the growing bump makes left-side sleeping increasingly necessary (optimal for blood flow to the placenta and kidneys), positional discomfort increases, the baby’s kicks become strong enough to wake you, heartburn worsens lying down, and the frequency of nighttime urination increases. What consistently helps:
- A full-length pregnancy pillow between the knees and supporting the belly significantly reduces the strain of side-sleeping
- Elevating the head of the bed 4–6 inches (or sleeping on a wedge pillow) reduces nighttime heartburn substantially
- Avoiding eating within 2 hours of bedtime minimizes both heartburn and the active digestion that can disrupt sleep
- Room temperature slightly cooler than usual — pregnant women run warm, and cooler environments improve sleep quality
- Short naps (20–30 minutes) in the afternoon, if circumstances allow, offset the nighttime sleep debt without significantly disrupting nighttime sleep
Nutrition at 24 Weeks — The Iron-Plus-C Strategy
With blood volume at peak expansion and iron deficiency anemia peaking at Week 24–28, iron + vitamin C pairing is the most impactful nutritional strategy this week. Non-heme iron (from plants) absorbs at only 2–20% without enhancement — but vitamin C increases non-heme iron absorption by up to 67% when consumed in the same meal.
| Nutrient | Why Critical at 24 Weeks | Best Sources + Strategy |
| Iron + Vitamin C | Blood volume at peak expansion — dilutional anemia worst this week! Iron deficiency = fatigue, breathlessness, palpitations. Critical for baby brain myelination continuing. | Beef/lentils + vitamin C in same meal! Spinach + lemon. Fortified cereals + OJ. Avoid tea/coffee within 1 hr of iron foods (inhibits absorption). |
| DHA Omega-3 | Brain cortical folding continuing + myelination accelerating. Taste bud neural connections being made. Eyes (retina layers forming) require DHA for photoreceptor development. | Cooked salmon 2x/week, sardines, DHA-fortified eggs, walnuts, chia. DHA supplement 200-300mg if fish limited. |
| Calcium + Vit D | Baby skeleton mineralizing, dental buds forming. Lung capillary network development. If calcium intake low, baby draws from maternal bone stores. | Dairy, fortified plant milk, sardines with bones, tofu, greens. Vitamin D supplement 1000-2000 IU (discuss with OB). |
| Fiber + Water | Iron supplements commonly cause constipation — fiber essential. Heartburn management via small frequent meals. Swelling managed by adequate hydration. | 25-30g fiber. 8-10 glasses water. Prunes, oats, pears, legumes. Small meals, eat slowly, stay upright. |
| Folate | Neural tube is closed, but folate continues supporting rapid brain growth and new cell production throughout pregnancy. Reduces neural complication risk. | Leafy greens, lentils, asparagus, fortified grains. Prenatal vitamin folic acid (check your brand dose — 600-800mcg/day target). |
Consider that your prenatal vitamin’s iron level matters significantly this week. Most standard prenatal vitamins contain 27mg of iron — the recommended daily amount for pregnancy — but women with established deficiency often need 45–60mg supplemental iron (in split doses with vitamin C). Review your prenatal vitamin’s iron content and discuss whether additional supplementation is appropriate with your OB at the Week 24 appointment. Our best prenatal vitamins guide covers which formulations offer the most bioavailable iron forms.
For Your Partner — Week 24 Actions
- Accompany her to the GD screening if possible: The glucose challenge test is a routine appointment that lasts about 90 minutes (time for the wait, the drink, the one-hour wait, and the blood draw). Having a partner there makes the wait less tedious, provides support if she’s anxious about the result, and keeps the experience lighter. More importantly: if the result comes back requiring the 3-hour OGTT, a supportive presence at the follow-up matters significantly.
- Understand GD together: If gestational diabetes is diagnosed, the management plan involves dietary changes that affect the household’s eating patterns — lower-glycemic meals, controlled carbohydrates, regular meal timing. A partner who understands why the changes are necessary and participates in making them (rather than bringing home donuts) makes compliance dramatically easier and the experience less isolating. GD is common (approximately 6–7% of US pregnancies), manageable, and not a failure — understanding it as a shared logistical challenge rather than a source of stress makes an enormous difference.
- Iron and meals: With iron deficiency anemia peaking this week, energy levels may be noticeably lower and breathlessness more common. This is a good week to take on more of the cooking (if possible), specifically making iron-rich meals paired with vitamin C: steak or beef stir-fry with broccoli and bell peppers; lentil soup with tomatoes; spinach salad with citrus dressing. The nutritional strategy that helps most right now is practical, not supplemental.
- Hospital tour — book it this week: Third trimester begins in three weeks. The prenatal tour of the labor and delivery unit should be booked now so you can visit before Week 32 or 33. Walk the floor: labor rooms, delivery suite, recovery, NICU location (just to know where it is — knowledge reduces fear of the unknown), parking, entrance, registration. A hospital bag checklist for mom is your next reading assignment — start gathering items.
- Read the viability table together: If she has been carrying any quiet anxiety about viability week, reading the survival rates table together — understanding what the numbers actually mean, what the NICU options are, what factors affect outcomes — is a better response than deflection or false reassurance. Being informed together is more calming than uncertainty navigated alone.
When to Call Your Doctor at 24 Weeks Pregnant
- Regular contractions before Week 37: Four or more in one hour, especially if not stopping with rest and hydration — same-day OB contact.
- Pelvic pressure or the feeling baby is pushing down: New or worsening sensation — same-day evaluation for preterm labor.
- Changes in vaginal discharge: Watery, bloody, or mucus-like before Week 37 — same-day evaluation.
- Fever above 100.4°F / 38°C: Contact your OB.
- Unusual fatigue, breathlessness, or heart palpitations: Could indicate significant iron deficiency anemia — report at your Week 24 prenatal visit or sooner if severe.
- Sudden facial or hand swelling + headache + vision changes: Possible preeclampsia — urgent OB contact.
- Decreased fetal movement: If regular kicks have gone quiet — lie on your left side, count movements for one hour. Fewer than 10 movements in a consistent kicker — contact your OB.
- Round ligament pain that is rhythmic, crampy, or accompanied by any discharge: Distinguished from normal round ligament pain (brief, movement-triggered, stops quickly) — atypical presentations require evaluation.
Your Week 24 Pregnancy Checklist
- ☑ 🩺 GD SCREENING — book and attend glucose challenge test this week!
- ☑ 🌽 Talk, sing, read to baby — voice recognition AND now taste exposure!
- ☑ 💊 Prenatal vitamin daily — check iron content with OB this week
- ☑ 🥩 Iron-rich meals DAILY + vitamin C in same meal — anemia peak this week!
- ☑ 🐟 DHA-rich meal — salmon, sardines (retina + brain layers forming)
- ☑ 🏋️ Pelvic floor exercises — 3×10 every single day
- ☑ 🏥 Hospital tour — BOOK THIS WEEK (third trimester in 3 weeks!)
- ☑ 👜 Hospital bag checklist — begin gathering items now
- ☑ 🛌 Pregnancy pillow + elevated head of bed for sleep and heartburn
- ☑ 📸 Weekly bump photo — the viability week photo is worth taking
- ☑ 💧 8-10 glasses water + 25-30g fiber (extra important with iron supplementation)
- ☑ 🌿 Slow down movements — bend from knees, stand slowly, roll onto side first
Frequently Asked Questions — 24 Weeks Pregnant
What does viability at 24 weeks actually mean?
Viability at 24 weeks means your baby could survive outside the womb with intensive NICU support. Survival rates at 24 weeks in US facilities range from approximately 42–70%, depending on the quality of the NICU, birth weight, the baby’s individual development, and other clinical factors. Viability is not a guarantee — it is a threshold where intensive intervention has a meaningful chance of success. Survival probability increases 2–4% per day between Weeks 23–26. Reaching Week 24 is significant, but staying in the womb through Week 28, 32, 36, and 40 is dramatically better for outcomes at every step.
What is the glucose challenge test and how do I prepare?
The glucose challenge test (GCT) is the standard screening for gestational diabetes at Weeks 24–28. No fasting is required — eat normally beforehand. At the appointment: you drink a 50g glucose solution, wait exactly one hour (sitting), and have one blood draw. If your glucose is below 140 mg/dL, you’ve passed — no GD. If it’s 140 or above, you proceed to the 3-hour OGTT, which determines whether you actually have GD. Approximately 15–25% of women who need the 3-hour test pass it without a GD diagnosis. One number on the 1-hour screen is not a diagnosis.
Can my baby taste food at 24 weeks?
Yes — taste buds are fully formed and functional at 24 weeks. Flavor compounds from the foods you eat cross the placenta into the amniotic fluid, which the baby swallows approximately 400–500ml of daily. The now-complete taste system detects these flavors. Research shows that babies show preferences for flavors experienced prenatally — babies born to mothers who regularly ate vegetables during pregnancy accept vegetables more readily during weaning. Eating a varied, flavorful diet through the second half of pregnancy introduces your baby to the food landscape of their culture and family.
When will my baby’s eyes open?
The eyelids, which have been sealed shut since early in the second trimester to protect the developing cornea and retina, will begin to open at approximately Week 26–28. The cornea is developing its full structure at Week 24, and the retina’s layers are maturing. Once open, the baby will be able to detect light and dark — the flashlight trick (holding a bright light against the belly) works from about Week 26–28 onward. Full visual development continues through the first year after birth.
What is round ligament pain and is it dangerous?
Round ligament pain is a sharp, brief twinge felt on one or both sides of the lower abdomen, triggered by fast movements like rolling over in bed, standing quickly, sneezing, or coughing. It is caused by the rapid stretching of the round ligaments — the cord-like structures that support the growing uterus. It is completely normal and not dangerous. Management: move slowly and deliberately when changing positions, use a support belt, and apply a heating pad (low setting) to the area. Contact your OB if you have pain that is rhythmic, persistent, crampy, or accompanied by discharge or pressure — that is different from round ligament pain.
Why am I so tired at 24 weeks pregnant?
Fatigue at 24 weeks has a specific medical explanation beyond general pregnancy exhaustion: blood volume is at peak expansion right now (40–50% above pre-pregnancy), and the dilutional effect — more plasma than red blood cells — means iron deficiency anemia is most common and most symptomatic at Weeks 24–28. Breathlessness, heart palpitations, and disproportionate fatigue are often the result. Your OB will check hemoglobin at the Week 24 visit; supplemental iron (with vitamin C) can address genuine deficiency. Sleep disruption from positional discomfort, nighttime urination, and baby kicks also compounds the fatigue. Address the iron first — the other causes are managed with sleep hygiene.
Is linea nigra normal?
Yes — linea nigra is completely normal and affects the majority of pregnant women. It appears as a dark vertical line running from the navel down to the pubic area (and sometimes upward toward the ribs) caused by the same pregnancy hormones responsible for other pigmentation changes. It requires no treatment, is harmless, and typically fades within several months after delivery. Sun protection reduces intensity during pregnancy.
💗 The Emotional Reality of Week 24 — You Made It Here
The word ‘viable’ is in your chart now.
For some women, reaching Week 24 carries enormous weight — a pregnancy fought for, a loss survived, a fear that has lived quietly since the first trimester that can now, fractionally, release. For others, Week 24 is simply another week, the viability conversation an abstraction that doesn’t speak to their experience. Both are completely fine. Both are real.
What Week 24 offers, practically: the knowledge that the baby you’ve been building is real to the outside world now in a medical sense. That if something happened — something you cannot control — there is a conversation to be had, a set of choices to be made, a team of neonatologists trained for exactly this. You are not alone in that.
And week by week, the numbers improve. The surfactant increases. The lungs branch further. The eyes prepare to open for the first time. The baby swallowing amniotic fluid learns the flavors of your kitchen — tasting today what you ate for lunch. None of this is small.
Eat something good this week. Your baby is tasting it with you. 💗
👶 What’s Next — 25 Weeks Pregnant Preview
25 Weeks Pregnant brings the baby past the viability threshold with improving odds, and introduces brand-new developments worth knowing:
- 🌽 Large corn — ~34.6cm, ~660–700 grams
- Eyes beginning to open in the first days of the Week 25–28 window!
- Capillaries visible under the still-thin skin — giving a pink-red glow
- Hair begins growing on the head — texture and color determined but not yet visible outside
- Hands increasingly strong — grip reflex more powerful each week
- Brain’s wrinkled cortex expanding as skull bones soften at sutures for delivery
Follow our complete pregnancy week by week guide as you move through the final weeks of the second trimester and toward the threshold of the third. Every week from here is a week worth celebrating. 💗
Week 24: The Corn That Can Taste Your Cooking
At 24 weeks pregnant, you are carrying a viable baby who is tasting the flavors of your kitchen, learning the light-dark rhythm of your days through closed eyelids that are preparing to open, accumulating the early stool that will be passed in the first hours of life, and breathing in practice through a diaphragm building toward the moment it will do this for real. The viability threshold is not the finish line — it is the bottom rung of a long ladder. But it is a rung you have now climbed past.
For everything still ahead, our pregnancy tips for first time moms is alongside you from this week through the end. The third trimester is three weeks away. The baby is cooking. 🌽💗


1 thought on “24 Weeks Pregnant: Viability, Baby Size, GD Screening & Symptoms”