Something is happening inside your baby’s body right now that may be setting labor in motion.
Your baby’s adrenal glands have been building toward a cortisol surge for weeks. At 37 weeks pregnant, that cortisol reaches the level needed to trigger a shift in the placenta’s hormone production – moving away from progesterone, which maintains pregnancy, and toward estrogen and prostaglandins, which prepare the cervix and uterus for labor. Your baby is not a passive passenger waiting to be delivered. Your baby is signaling its own readiness.
The brain that has been developing since Week 3 will also continue developing well after birth. At 37 weeks pregnant, your baby’s brain weighs roughly two-thirds of what it will weigh at one year old. By age two, it will weigh three times what it weighs today. The most rapid brain development of your child’s entire life is still ahead – which is why nutrition, sleep, and stimulation in the first two years matter so much.
And the waxy vernix that has protected your baby’s skin for months is doing something new this week. As amniotic fluid volume continues to decline, vernix particles that shed from your baby’s skin are not being replaced – they are dissolving back into the fluid. By the time most full-term babies arrive, little vernix remains. What does remain is still protective and worth leaving in place.
Three weeks from your due date. Here is everything happening at 37 weeks pregnant.
Contents
- 1 Quick Summary: 37 Weeks Pregnant
- 2 Is 37 Weeks Full Term? The Answer Most Guides Get Wrong
- 3 What’s Happening in Your Body at 37 Weeks Pregnant
- 4 Baby Development at 37 Weeks Pregnant
- 5 What Actually Triggers Labor – The Biology Nobody Explains
- 6 37 Weeks Pregnant Symptoms
- 7 What to Know About Postpartum Depression – Prepare Now
- 8 The Prostaglandin Question – What Your Provider May Tell You
- 9 Nutrition at 37 Weeks Pregnant
- 10 Partner Tips for Week 37
- 11 37 Weeks Pregnant Checklist
- 12 Frequently Asked Questions – 37 Weeks Pregnant
- 12.1 What trimester is 37 weeks pregnant?
- 12.2 How many months is 37 weeks pregnant?
- 12.3 Is 37 weeks full term or early term?
- 12.4 How much does a baby weigh at 37 weeks pregnant?
- 12.5 What triggers labor at 37 weeks?
- 12.6 What is the difference between baby blues and postpartum depression?
- 12.7 Why is my baby so still at 37 weeks pregnant?
- 13 Looking Ahead: 38 Weeks Pregnant
Quick Summary: 37 Weeks Pregnant
| Detail | Info |
| Baby size | Swiss chard / winter melon – ~48-49 cm, ~2.9-3.2 kg (6.3-7 lbs) |
| Trimester | Third trimester – Week 10 of T3 |
| Term status | EARLY TERM (not full term – full term begins Week 39) |
| Weeks remaining | ~3 weeks to due date |
| Top milestone | Baby’s cortisol triggers labor hormone shift + brain doubles by year 1 |
| This week’s action | Understand what triggers labor + prepare for postpartum |
Is 37 Weeks Full Term? The Answer Most Guides Get Wrong
This is perhaps the most important thing to understand at 37 weeks pregnant – and it is one of the most consistently misrepresented facts in pregnancy content.
The NHS website calls 37 weeks ‘full term.’ Many pregnancy apps use the same language. It feels logical – you are three weeks from your due date, your baby is a healthy weight, the lungs are functional. Surely that is full term.
It is not. In 2013, the American College of Obstetricians and Gynecologists and the Society for Maternal-Fetal Medicine formally reclassified pregnancy timing after research showed measurable differences in outcomes between 37-38 week births and 39-40 week births. Their current classification:
| Classification | Weeks | Key Implications |
| Preterm | Before 37 weeks 0 days | Significant organ immaturity – NICU standard |
| Early Term | 37 weeks 0 days – 38 weeks 6 days | Looks full term, but brain connectivity + liver maturation incomplete |
| Full Term | 39 weeks 0 days – 40 weeks 6 days | Optimal outcomes – recommended window for planned delivery |
| Late Term | 41 weeks 0 days – 41 weeks 6 days | Post-dates monitoring intensifies |
| Post Term | 42 weeks and beyond | Placenta aging – induction typically recommended |
At 37 weeks pregnant you have entered early term. Your baby will almost certainly thrive if born now. But ‘early term’ is not the same as ‘full term’ – and the difference matters particularly for brain development, liver enzyme maturation, and feeding ability.
The reason this distinction was made in 2013 is that hospitals were scheduling elective inductions and cesarean sections at 37-38 weeks, partly based on the old ‘full term at 37 weeks’ belief. The data showed these babies had higher NICU admission rates, more feeding difficulties, and more jaundice than babies born at 39 weeks. The language was updated to change clinical practice.
This is not cause for alarm if you are 37 weeks pregnant. Spontaneous labor at this stage is completely safe to proceed with. It simply means that elective, non-medically-indicated delivery before 39 weeks carries a real cost – and that every day your pregnancy continues from this point adds something real.
What’s Happening in Your Body at 37 Weeks Pregnant
At 37 weeks pregnant, the physical experience of pregnancy is reaching its most intense. Your uterus is at or near maximum size. Your baby is somewhere between 2.9 and 3.2 kg. Everything that was already uncomfortable at Week 30 has been amplifying weekly since then.
Weekly appointments continue from this point. At each visit, your provider will check blood pressure, urine protein, fundal height, baby’s heartbeat, and baby’s position. Many providers will also offer a cervical exam – optional, and not predictive of labor timing, but some women find the information useful.
You may be on maternity leave now or approaching it. If you are, the temptation is to fill the time with preparations – and some preparation is genuinely useful. But sleep, rest, and anything that reduces physical strain is equally valuable right now. Your body is building toward something significant. Reserve energy for it.
What to expect at your Week 37 appointment:
- Blood pressure, urine protein, fundal height
- Baby’s heartbeat
- Baby’s position – 95% of babies are head-down by Week 37
- Optional cervical exam – effacement and dilation
- Discussion of induction – timing, criteria, and your preferences
- Signs of labor review – what to watch for and when to go to hospital
- Confirmation that hospital bag is in the car
Baby Development at 37 Weeks Pregnant
At 37 weeks pregnant, your baby measures approximately 48-49 cm from head to heel and weighs around 2.9 to 3.2 kg – roughly the size and weight of a large bunch of Swiss chard or winter melon.
| Detail | Measurement |
| Length | ~48-49 cm (about 19 inches) |
| Weight | ~2.9-3.2 kg (approx. 6.3-7 lbs) |
| Size comparison | Swiss chard / large leek / winter melon |
| Heart rate | 110-160 bpm |
| Brain status | ~2/3 of 1-year weight – will double by year 1, triple by year 2 |
Key developments this week:
- Cortisol surge triggering labor readiness: Your baby’s adrenal glands are producing cortisol at levels high enough to begin shifting the placenta’s hormone balance – increasing estrogen and prostaglandins while decreasing progesterone. This is the biochemical signal that initiates the cascade leading to labor. Your baby is participating in its own delivery.
- Vernix dissolving into amniotic fluid: As amniotic fluid volume continues declining and as your baby fills more of the available space, vernix particles that shed from the skin dissolve back into the fluid rather than accumulating. Most full-term babies have little visible vernix at birth – those born slightly early tend to have more.
- Brain: only a fraction of its final size: Your baby’s brain at 37 weeks weighs approximately 400 grams. By one year old, it will weigh approximately 900 grams. By age two, approximately 1,100 grams. The brain your baby is born with is not the finished product – it is the foundation. The connections formed in the first two years of life are shaped by everything experienced after birth.
- Grasp reflex fully developed: Your baby can grip firmly. The grasp reflex tested in every newborn examination – the response to a finger placed in the baby’s palm – is fully operational. At birth, the grip is strong enough that a baby can briefly support its own weight.
- Sucking and swallowing fully coordinated: The suck-swallow-breathe coordination needed for feeding is complete. When placed skin-to-skin after birth, most babies make their way to the breast instinctively within the first hour – the breast crawl is driven in part by the olfactory recognition of familiar scent compounds, and in part by this coordinated reflex.
- Circulatory and musculoskeletal systems complete: The heart, blood vessels, and entire skeletal-muscular system are fully developed. The circulatory changes that occur at birth – the ductus arteriosus closing, the foramen ovale sealing, blood redirecting through the lungs – are ready to happen the moment the first breath is taken.
- Fingernails past fingertips: Fingernails extend beyond the fingertip ends. Some babies scratch themselves in utero at this stage. Baby nail files (not clippers) are the safest trimming tool in the first weeks of life.
What Actually Triggers Labor – The Biology Nobody Explains
Most pregnancy guides describe the signs of labor – contractions, water breaking, mucus plug. Almost none explain what triggers labor in the first place. The mechanism is not fully understood even in obstetric research, but here is what is known.
Labor initiation is not a single event. It is a cascade – a series of hormonal and mechanical changes that build on each other over days or weeks before contractions become strong and regular.
| Step | What Happens | Who or What Drives It |
| 1. Cortisol surge | Baby’s adrenal glands produce high-level cortisol | Baby – signaling maturity and readiness |
| 2. Placental shift | Cortisol triggers the placenta to reduce progesterone and increase estrogen production | Placenta responding to baby’s cortisol signal |
| 3. Prostaglandin release | Rising estrogen stimulates prostaglandin production in the uterine lining and cervix | Uterine tissue |
| 4. Cervical ripening | Prostaglandins cause the cervix to soften, thin (efface), and begin to open (dilate) | Cervix responding to prostaglandins |
| 5. Oxytocin receptors multiply | Rising estrogen causes the uterus to develop more oxytocin receptors – becoming increasingly sensitive to oxytocin | Uterine muscle |
| 6. Contractions begin | Oxytocin – released from the pituitary gland and locally by the uterus – triggers the uterine contractions of labor | Brain + uterus working together |
| 7. Ferguson reflex | As the baby’s head presses on the cervix, this triggers more oxytocin release – a positive feedback loop that intensifies contractions | Baby’s head + cervix + brain |
This is why labor is self-sustaining once it starts – the Ferguson reflex creates a positive feedback loop. The more the head presses on the cervix, the more oxytocin is released, the stronger the contractions become, the further the head descends.
Synthetic oxytocin (Pitocin) used in induction works by entering this cascade at Step 6 – triggering contractions. Prostaglandin gels or inserts used for cervical ripening enter at Step 4. Understanding where intervention acts helps make sense of induction conversations with your provider.
37 Weeks Pregnant Symptoms
Pelvic Pressure and the Baby Drop
If your baby has engaged or is engaging this week, the shift in where you feel pressure is unmistakable. Upper body symptoms – heartburn, shortness of breath, the fullness after small meals – improve. Lower body symptoms intensify: lightning crotch, bladder urgency, pelvic heaviness, and a sensation of walking with something large settled deep in the pelvis.
Not all babies have dropped by 37 weeks – second and subsequent babies often do not engage until labor begins. The absence of dropping does not mean something is wrong. It means your pelvis and baby have a different timeline.
Anxiety and Emotional Intensity
Three weeks from your due date, the emotional landscape of pregnancy shifts for most women. The abstract anticipation of earlier months becomes immediate reality. Everything feels close.
Anxiety is extremely common at 37 weeks pregnant – about the birth itself, about the pain, about whether everything will be okay, about becoming a parent. Fear and excitement often coexist in the same moment. This does not mean something is wrong with your mental state. It means you are human and you understand what is coming.
What helps: talking to your partner or a close friend who will actually listen, walking outdoors when your body allows it, reducing time spent reading graphic birth stories online, and reminding yourself that the anxiety often peaks before labor begins and eases once it starts. Active labor tends to be so consuming that the mental energy available for anxiety disappears.
If anxiety is severe, persistent, or accompanied by feelings of hopelessness or disconnection, speak to your provider. Perinatal anxiety is a recognized and treatable condition – not a character weakness.
Spotting After Cervical Exam or Intimacy
Light spotting at 37 weeks pregnant is very common – particularly after a cervical exam or sexual intercourse. The cervix is highly vascularized (rich in blood vessels) and sensitive. Even gentle contact can cause a small amount of bleeding that appears on toilet paper or underwear as pink or brown spotting.
This is different from heavy bleeding or bleeding that resembles a period. Light spotting after contact is essentially always benign at this stage. Heavy or persistent bleeding warrants immediate contact with your provider.
Increased Braxton Hicks – Or Is It Real Labor?
Braxton Hicks at 37 weeks pregnant can be strong, frequent, and convincing. Many women at this stage have one or two experiences of contractions that feel genuinely significant – only to watch them gradually space out and disappear. This is sometimes called prodromal labor or false labor.
Prodromal labor is not a failure – it is the uterus rehearsing, the cervix beginning to change, the body incrementally progressing toward active labor over days or weeks. Women experiencing prodromal labor are not imagining it. The contractions are real. They are simply not yet the sustained, progressive pattern of active labor.
When in doubt, contact your provider or go in. At 37 weeks, your provider would rather assess you and send you home than have you wait alone uncertain.
Colostrum Leaking More Noticeably
Colostrum leakage tends to increase around Week 37 as hormonal changes intensify. Some women notice it on their clothing or bedsheets. Breast pads manage this comfortably. There is no need to try to express or collect colostrum before birth – it will be there when your baby needs it, and the quantities perfectly match a newborn’s stomach capacity on day one.
What to Know About Postpartum Depression – Prepare Now

The NHS specifically recommends learning about postpartum depression at Week 37 – and it is advice that most pregnancy guides skip entirely. Week 37 is the right time because you still have mental bandwidth to process this information, and because knowing the signs early dramatically improves outcomes.
Postpartum depression (PPD) is not the same as the baby blues – the weepiness and emotional rollercoaster that affects approximately 80% of new mothers in the first two weeks and resolves on its own. PPD is a more serious, persistent condition that requires support and often treatment.
| Baby Blues | Postpartum Depression | |
| When it starts | Days 2-5 after birth | Can begin anytime in the first year – often Week 2-8 |
| How common | ~80% of new mothers | ~10-15% of new mothers (partners too – ~10%) |
| Duration | Resolves within 2 weeks | Persists beyond 2 weeks – worsens without support |
| Symptoms | Tearfulness, mood swings, overwhelm, sensitivity | Persistent sadness, inability to bond, feeling like a bad mother, loss of interest, anxiety, thoughts of harm |
| What helps | Rest, support, time | Professional support, therapy, sometimes medication – always assessment first |
| Risk factors | N/A – affects most mothers | History of depression, difficult birth, lack of support, sleep deprivation, isolation |
Why Week 37 is the time to prepare:
- You can identify your risk factors now and discuss them with your provider
- Your partner can learn the signs – they may recognize PPD before you do
- You can identify a mental health contact to reach out to if needed – having this ready matters
- Understanding that PPD is not your fault and is not permanent reduces the shame barrier to seeking help
Postpartum depression is not a reflection of how much you love your baby. It is a medical condition driven by the dramatic hormonal shifts of delivery and the physical and emotional demands of new parenthood. It responds well to treatment – but only if it is identified.
Ask your provider about their postpartum mental health screening process. Most practices screen at 6 weeks postpartum – but symptoms can begin earlier. Know that you can contact your provider between appointments if you are struggling.
The Prostaglandin Question – What Your Provider May Tell You
At some point in the final weeks of pregnancy, you may hear advice about sexual intercourse being potentially helpful for labor. This is not folklore. It has a biochemical basis.
Semen contains prostaglandins – the same compounds involved in Step 3 of the labor cascade. When prostaglandins come into contact with the cervix, they can contribute to the cervical ripening process. This effect is modest and not sufficient to initiate labor in a cervix that is not already preparing – but it may nudge a cervix that is already beginning to ripen.
Whether to act on this information is entirely a personal decision. It requires a cervix that is not at risk of infection (intact membranes), a low-risk pregnancy, and consent from both partners. If your membranes have ruptured or you have placenta previa, this should not be attempted.
Some providers bring this up. Others do not. If you are curious, ask. The evidence is real – just modest.
Nutrition at 37 Weeks Pregnant
| Nutrient | Why It Matters at Week 37 | Daily Target and Sources |
| Protein | Baby still gaining ~8-12 oz/week and feeding readiness requires adequate protein reserves | 71g+ daily – chicken, eggs, Greek yogurt, lentils, cottage cheese, fish |
| Healthy fats | Brain fat composition is 60% fat – DHA and healthy fats in your diet directly build the brain your baby will be born with | Avocado, olive oil, nuts, fatty fish, full-fat dairy |
| Iron | Blood volume at maximum – iron deficiency at delivery increases postpartum hemorrhage risk and postpartum fatigue | Red meat, lentils, spinach + always paired with vitamin C |
| DHA (Omega-3) | Brain myelination continues – the neural connections forming right up to birth require DHA | Salmon, sardines, eggs, prenatal vitamins with DHA |
| Magnesium | Leg cramps peak – magnesium glycinate before bed improves sleep quality significantly | Almonds, pumpkin seeds, dark chocolate, supplements (ask provider) |
| Fiber + Water | Constipation and hemorrhoids at worst – hospital births often worsen both temporarily | Prunes, oats, beans, vegetables + 8-10 glasses water daily |
If appetite has improved since your baby dropped, take advantage of this window. Nutrient stores built now support your postpartum recovery – particularly iron levels, which affect both energy and breast milk production in the first weeks.
Partner Tips for Week 37
- Read about postpartum depression today – you may be the first person to recognize it, and you need to know what you are looking for
- Learn the Ferguson reflex concept – understanding that labor intensifies itself once it starts reduces the fear that ‘things are getting out of control’ during active labor
- Know the hospital logistics cold – parking, overnight entrance, where to go, who to call, how long the drive takes at 3am
- The hospital bag in the car is non-negotiable now – labor can begin any day
- If she is experiencing prodromal labor – regular-seeming contractions that stop – do not minimize it. These are real, they are exhausting, and they represent real progress
- Ask how she is doing emotionally. Week 37 carries a specific kind of weight – three weeks from a life-changing event, with no control over when it begins. Presence and listening matter more than practical problem-solving right now.
- Sleep while you can – genuinely. The sleep you get in the next three weeks is the reserve you will draw on in the first month with a newborn.
37 Weeks Pregnant Checklist
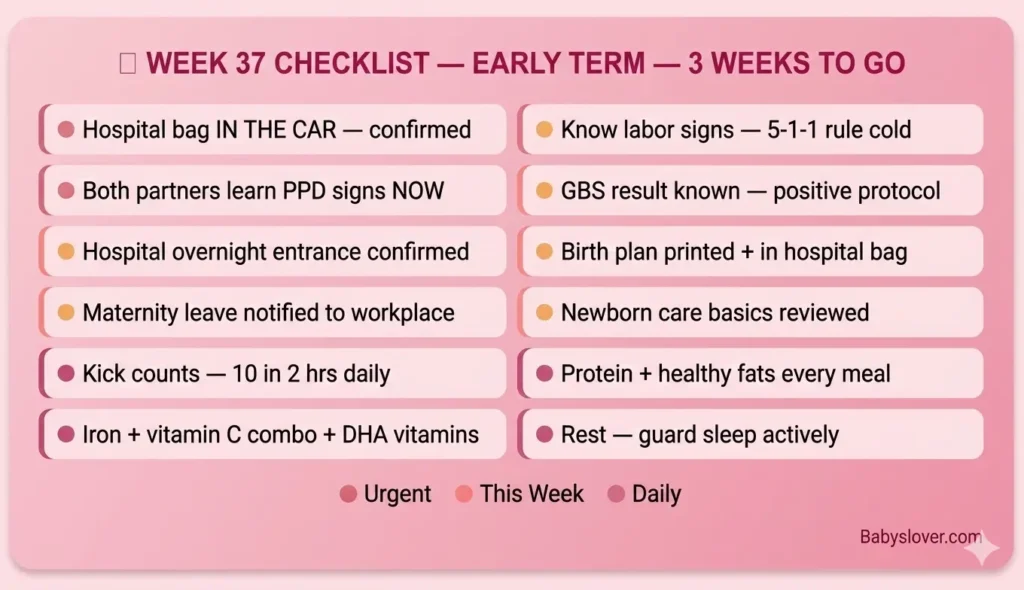

| Task | Priority |
| Hospital bag in the car – confirmed this week | URGENT |
| Know labor signs + 5-1-1 rule + go-immediately criteria | URGENT – know cold |
| Both partners learn postpartum depression signs this week | URGENT |
| Continue kick counts – 10 movements in 2 hours, daily | Daily |
| Know hospital directions + overnight entrance | Confirm this week |
| GBS result known – positive = arrive earlier for antibiotics | Confirm this week |
| Birth plan printed + in hospital bag | Confirm this week |
| Maternity leave logistics – notify workplace if not done | This week |
| Newborn care basics reviewed – first bath, cord care, safe sleep | This week |
| Breastfeeding preparation – nursing bra, lanolin cream, nursing pillow ready | This week |
| Identify postpartum support contact if needed | This week |
| Protein + healthy fats at every meal | Daily |
| Iron + vitamin C + DHA prenatal vitamins | Daily |
| Magnesium before bed if leg cramps are disruptive | Daily if needed |
| Rest – guard your sleep actively | Daily |
Follow our pregnancy week by week guide for every development from now to delivery.
Frequently Asked Questions – 37 Weeks Pregnant
What trimester is 37 weeks pregnant?
37 weeks pregnant is the tenth week of the third trimester. Third trimester runs from Week 28 through Week 40. You have approximately 3 weeks remaining until your due date.
How many months is 37 weeks pregnant?
At 37 weeks pregnant, you are 9 months pregnant. Full-term pregnancy is 40 weeks, spanning approximately 9.5 calendar months. Most people reach their due date between 9 and 10 months after their last menstrual period.
Is 37 weeks full term or early term?
37 weeks is early term – not full term. The American College of Obstetricians and Gynecologists (ACOG) reclassified pregnancy timing in 2013 after research showed measurable outcome differences. Early term is Weeks 37-38. Full term is Weeks 39-40. Some sources (including the NHS) still use the older ‘full term at 37 weeks’ language, but ACOG’s current clinical definition is clear: full term begins at 39 weeks. A baby born at 37 weeks will likely do well – but the two additional weeks to 39 carry real developmental benefits, particularly for brain connectivity and liver function.
How much does a baby weigh at 37 weeks pregnant?
At 37 weeks pregnant, your baby weighs approximately 2.9 to 3.2 kg (about 6.3 to 7 lbs) and measures around 48-49 cm from head to heel – roughly the size of a large bunch of Swiss chard or leek. Baby continues gaining approximately 8-12 oz per week until birth.
What triggers labor at 37 weeks?
Labor is triggered by a cascade that begins with your baby’s own cortisol production signaling readiness. Baby’s cortisol shifts the placenta’s hormone balance, increasing prostaglandins that ripen the cervix and estrogen that multiplies oxytocin receptors in the uterus. Once the uterus becomes sensitive enough to oxytocin and the cervix is sufficiently ripened, contractions begin. The Ferguson reflex – the baby’s head pressing on the cervix releasing more oxytocin – then creates a positive feedback loop that sustains and intensifies labor.
What is the difference between baby blues and postpartum depression?
Baby blues are very common (affecting ~80% of new mothers) and resolve within two weeks without treatment. They involve tearfulness, mood swings, and emotional sensitivity in the first days after birth. Postpartum depression is more serious, affects approximately 10-15% of new mothers (and ~10% of partners), begins anytime in the first year, and persists without support. Symptoms include sustained sadness, difficulty bonding, feeling like a bad parent, loss of interest, and sometimes intrusive thoughts. It is a medical condition that responds well to treatment – but only if identified. Week 37 is the time to learn the signs.
Why is my baby so still at 37 weeks pregnant?
Movement changes at 37 weeks pregnant as your baby fills most of the available space. You will likely feel fewer large kicks and more rolls, stretches, and position shifts. The type of movement changes – the frequency should not drop significantly. Continue daily kick counts (10 movements in 2 hours). If you notice a genuine decrease from your baby’s usual movement pattern, contact your provider. Do not wait until the next morning.
Looking Ahead: 38 Weeks Pregnant
At 38 weeks pregnant, your baby’s head and abdomen are approximately the same circumference – a milestone of proportional development. The brain continues building connections. Fat is still accumulating. And the labor cascade that may have already quietly begun is drawing closer to the threshold that produces regular, progressive contractions.
Three weeks. A baby participating in its own delivery. A brain that will keep growing for two more years. Keep going.