Two weeks from now, your baby crosses the threshold of viability.
That sentence deserves a moment. At Week 24 — two weeks from where you are right now — the medical community formally recognizes a gestational age at which survival outside the womb becomes possible with intensive care. The odds at 24 weeks are not favorable; the NICU journey is long and demanding. But the threshold exists. Right now, at 22 weeks pregnant, you are two weeks from that line.
The developmental reason that Week 24 matters — and why it doesn’t yet — is a substance called surfactant, and your baby’s lungs are beginning to produce it this week. Surfactant is the soap-like coating that allows the lung’s air sacs to inflate and stay open after each breath instead of collapsing. Without adequate surfactant, breathing air is not just difficult — it’s functionally impossible in a sustained way. At Week 22, production has begun in tiny amounts. It won’t be sufficient for unassisted breathing for several more weeks. But the factory has opened.
Week 22 also brings a grip reflex strong enough to grab and hold the umbilical cord — captured on detailed ultrasound with remarkable frequency. The eye color your baby is born with — or rather, the eye color that will develop in the first year — is not yet set: the irises have no pigment at Week 22. Pregnancy gingivitis is peaking for many women, a hormonal gum condition that the dentist needs to know about. And a small, joyful discovery: if you shine a flashlight at your belly, you may feel your baby move in response. At Babyslover, here is everything about 22 weeks pregnant: the surfactant explained in full, the viability conversation, and everything developing this week.
Just read last week? Our 21 weeks pregnant guide covered digestive enzymes, the baby-heavier-than-placenta milestone, and gestational diabetes screening prep.

| 📋 Quick Summary — Week 22 of Pregnancy | |
| Week | Week 22 of 40 — Second Trimester, Week 10 |
| Baby Size | 🌽 Corn (ear of corn) — ~28cm head-to-heel (11 inches) |
| Baby Weight | ~460 grams (about 1 pound!) |
| KEY MILESTONES | ✊ GRIP REFLEX — strong enough to grab umbilical cord! • 🫁 SURFACTANT BEGINS — lung coating production starts! • 👁️ EYE COLOR NOT SET — irises have zero pigment at Week 22 • 🔦 Reacts to light — flashlight test! • 🦷 Pregnancy gingivitis peaks • Testes beginning descent in males |
| Viability Note | ⏳ Week 24 — viability threshold — is just 2 weeks away. Understanding what viability means, and what it doesn’t, is an important Week 22 conversation. |
| Symptoms | Pregnancy gingivitis (swollen, bleeding gums), round ligament pain, hemorrhoids possible, back pain intensifying, heartburn, leg cramps, Braxton Hicks, skin itchiness continuing, increased sweating |
| Coming Up | 🩺 Gestational diabetes screening in just 2 weeks (Weeks 24-28) — confirm with OB now! | 🎯 Viability week 24 approaches — understanding the milestone |
Contents
- 1 🌱 Baby Development at 22 Weeks Pregnant
- 2 ⏳ Viability at Week 24 — The Conversation Worth Having
- 3 What’s Happening in Your Body at 22 Weeks Pregnant
- 4 What to Eat at 22 Weeks Pregnant — Calcium for the Surfactant Factory
- 5 For Your Partner — Week 22 Meaningful Actions
- 6 When to Call Your Doctor at 22 Weeks Pregnant
- 7 Your Week 22 Pregnancy Checklist
- 8 Frequently Asked Questions — 22 Weeks Pregnant
- 9 💗 The Emotional Reality of Week 22 — Two Weeks From a Threshold
- 10 👶 What Happens Next — 23 Weeks Pregnant Preview
- 11 Week 22: The Corn That Learned to Grip
🌱 Baby Development at 22 Weeks Pregnant
At 22 weeks pregnant, your baby measures approximately 28cm head-to-heel — the length of an ear of corn — and weighs about 460 grams, crossing the one-pound mark. The skin is still thin, reddish, and visibly wrinkled — there isn’t yet enough subcutaneous fat to smooth it out — and blood vessels are visible through it, giving the characteristic red-tinged appearance of second-trimester fetal skin. The face is increasingly complete: lips are becoming more distinct, eyebrows are defined, and all the structures of the eyes are formed. But there is a detail about those eyes that surprises most parents: they have no color yet.
| 🌱 Baby Development at 22 Weeks Pregnant | |
| Baby Size | 🌽 Corn — ~28cm head-to-heel (11 inches) |
| Weight | ~460 grams (1 pound!) — skin thin, reddish, wrinkled |
| KEY MILESTONE | ✊ GRIP REFLEX activated — baby can grasp and hold the umbilical cord. Nervous system mature enough to maintain grip. |
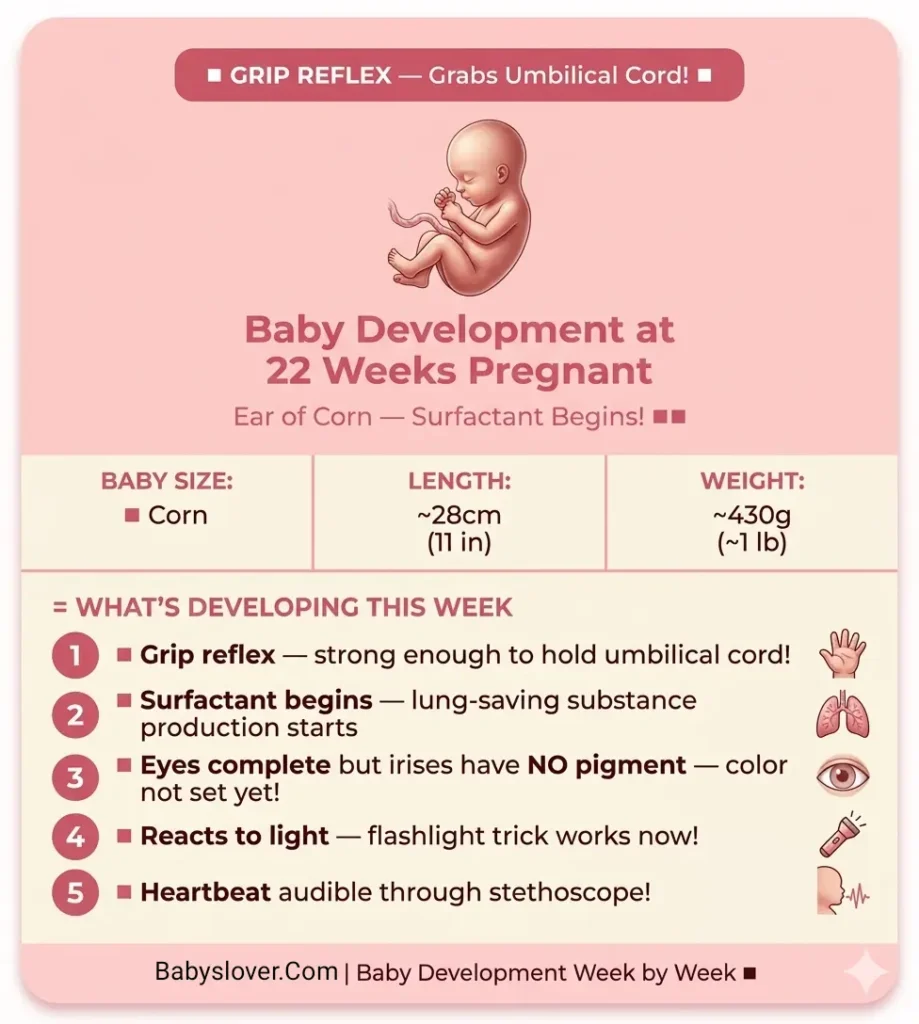
What Is Developing at Week 22
- ✊ Grip reflex — strong enough to hold the umbilical cord: The grip reflex is one of the most ancient and robust of all human reflexes — present at birth and persisting for several months, it is the reflex that causes a newborn’s fingers to curl around anything placed in the palm. At Week 22, this reflex has reached sufficient strength for the baby to grab and maintain hold of the umbilical cord, its own hands, its ears, and other nearby structures in the uterus. On detailed 3D/4D ultrasound performed around this time, the baby is frequently seen holding the umbilical cord — sometimes quite firmly. The grip reflex at this stage is not voluntary or conscious; it is a spinal cord-mediated reflex response to palmar contact. But the neural circuitry that will eventually become the voluntary, cortically controlled grip of a child catching a ball is the same system now being built and tested through these reflex activations.
- 🫁 Surfactant production begins — the lung-saving substance: Surfactant is a soap-like substance produced by specialized cells called type II pneumocytes that line the lungs’ air sacs (alveoli). Its function is mechanical: it reduces the surface tension of the fluid lining the alveoli, preventing the sacs from collapsing completely after each exhale. Without adequate surfactant, the effort required to re-inflate collapsed alveoli with each breath is so great that sustained breathing is not physiologically possible. This is exactly what happens in respiratory distress syndrome (RDS) — the primary cause of mortality in premature babies born before surfactant production is sufficient. At Week 22, the type II pneumocytes have begun producing surfactant, but only in tiny amounts — far below what’s needed for breathing air. Production increases progressively through the third trimester, reaching sufficient levels for most babies around Week 34-36 for normal breathing, with adequate amounts for survival with support appearing around Week 24-28. This is precisely why Week 24 is the viability threshold — not because other organs are ready, but because just enough surfactant exists for the lungs to be kept open with medical support.

💡 Synthetic surfactant is now given to premature babies in NICUs — one of the most life-saving treatments in neonatal medicine. Before synthetic surfactant was developed in the 1980s, respiratory distress syndrome was one of the leading causes of premature infant death. Today, premature babies born at 24 weeks can receive a dose of synthetic surfactant within the first hours of life, directly addressing the lungs’ inability to produce it on their own. The surfactant your baby is beginning to make at Week 22 is the same substance. 🫁
- 👁️ Eye color not set — irises have no pigment: At Week 22, the eyes are structurally complete — the cornea, lens, retina, and all optical components are formed and in place. But the irises contain essentially no melanin pigment at this stage. Melanin is the pigment that gives eyes their color — the more melanin, the darker the color, from pale blue at the lowest levels to dark brown at the highest. At birth, most babies have gray-blue or blue eyes because the iris has minimal pigment regardless of what the ultimate eye color will be. Eye color develops in the months after birth as melanin production in the iris increases in response to light exposure — the final eye color typically stabilizing between 6 and 12 months of age, though in some children it continues shifting until age 3. The eye color your baby will have as a child and adult is genetically determined but not yet expressed at Week 22.
- 🔦 Reacts to light — the flashlight trick: Although the eyelids are still fused, the retina is sufficiently developed at Week 22 that the baby can detect changes in light intensity through the abdominal and uterine walls. A bright light shone against the belly may cause the baby to turn away or become active in response. Many women enjoy this as a form of early interaction — shining a flashlight at the lower abdomen during an active period and noting the responding movement. The light reaching the baby is diffused and reddish by the time it passes through skin and uterine tissue, but the intensity change is detectable.
- 🧒 Male testes beginning descent: In male babies, the testes — which formed near the kidneys in the abdomen — begin their descent toward the scrotum around Week 22-26. This process, guided by a ligament called the gubernaculum, takes several weeks and is typically complete by Week 32-35, though some babies are born with undescended testes (cryptorchidism) that descend in the first year of life.
- 🎶 Heartbeat now audible with a stethoscope: By Week 22, the fetal heartbeat is loud enough to be heard through a standard stethoscope placed on the abdomen — not just on a Doppler device. This is a moment that partners often experience for the first time at this gestation, and it’s meaningfully different from hearing the heartbeat on medical equipment: it’s just a stethoscope, a belly, and a heartbeat at approximately 120-160 beats per minute.
💡 Fun fact: Shine a flashlight at your belly during an active period and you may feel your baby shift or kick in response. The baby can detect the intensity change through the abdominal and uterine walls even though the eyelids are still fused. The light reaching the baby is reddish and diffused — but the change in brightness is perceptible to the developing retina. 🔦
⏳ Viability at Week 24 — The Conversation Worth Having
Viability — the gestational age at which a baby may survive outside the womb with medical support — is widely cited as Week 24. With two weeks until that threshold from your current position at Week 22, it’s worth understanding what viability actually means, and what it doesn’t, so the word doesn’t carry more weight than it should.
What Week 24 Viability Actually Means
Week 24 is the generally accepted lower limit of viability, meaning that some babies born at 24 weeks can survive with intensive care. The survival rate at exactly 24 weeks is approximately 40-70% depending on the NICU, and the survivors face significant risks of long-term complications — chronic lung disease, neurological impairment, vision and hearing problems — because so many organ systems are still in critical development. Survival rates rise sharply with each additional week of gestation from Week 24 onward.
| Gestational Age | Approximate Survival | Context |
| 22 weeks | Extremely rare | Surfactant present in tiny amounts; lung development insufficient |
| 23 weeks | ~15-30% | Improving surfactant; some NICUs offer support |
| 24 weeks | ~40-70% | Viability threshold — NICU support required; significant risks remain |
| 26 weeks | ~80%+ | Survival significantly more likely; long-term outcomes improving |
| 28 weeks | ~90%+ | Dramatically better outcomes; lung development approaching functional |
| 34+ weeks | ~98-99% | Near-term; outcomes close to full-term with brief NICU if needed |
What viability does not mean: that a Week 24 birth is fine, or manageable, or expected to go well. It means the threshold has been crossed at which survival becomes possible — not likely, not easy, not without enormous medical support and significant risk of long-term complications. Every week from 22 to 40 is irreplaceable. The viability conversation is not cause for anxiety — it’s cause for appreciation of exactly where you are, and what each coming week is building toward.
What’s Happening in Your Body at 22 Weeks Pregnant
🦷 Pregnancy Gingivitis — The Dentist Visit You Need This Week
Pregnancy gingivitis — inflammation of the gums caused by pregnancy hormones — affects approximately 60-75% of pregnant women and is most commonly noticed in the second trimester when estrogen and progesterone levels are at their highest. The hormones increase blood flow to the gum tissue and alter the immune response in ways that make the gums more reactive to the bacteria in dental plaque. Symptoms: gums that are swollen, redder than usual, tender, and bleed when brushing or flossing — sometimes significantly even with gentle brushing. Management: brushing twice daily with a soft-bristled toothbrush in gentle circular motions, flossing daily (even if it causes some bleeding — stopping flossing makes gingivitis worse, not better), using alcohol-free antibacterial mouthwash, and seeing a dentist for a professional cleaning if you haven’t already this pregnancy. Tell your dentist you’re pregnant — they can adjust their approach, avoid X-rays except when essential, and use pregnancy-safe products. Untreated periodontal disease in pregnancy has been associated in some research with preterm birth and low birth weight, though causation is still debated. Either way: the dentist visit is worth having.
😣 Round Ligament Pain — The Sharp Twinges Explained
Sharp, stabbing, or pulling pains in the lower abdomen or groin — round ligament pain — are extremely common from the second trimester onward. The round ligaments are thick fibrous bands that run from the top of the uterus down through the groin, holding the uterus in position. As the uterus grows and its weight increases, these ligaments are under constant stretching stress. Sudden movements — rolling over in bed, standing up quickly, sneezing, laughing, coughing — cause a rapid tensing of the already-stretched ligament that produces a sharp, often brief pain on one or both sides. Round ligament pain is harmless and requires no treatment. Management: moving more slowly and deliberately when changing position, supporting the belly when coughing or sneezing, and applying a heating pad at low setting to the affected area. If pain is severe, persistent (lasting more than a few minutes), or accompanied by other symptoms (fever, bleeding, urinary symptoms), contact your OB to rule out other causes.
😰 Hemorrhoids — Why They Develop and What Actually Helps
Hemorrhoids — swollen, enlarged veins in the rectal area — become increasingly common from the second trimester onward, driven by the same circulatory mechanics as varicose veins: increased blood volume, the growing uterus pressing on pelvic veins, and relaxin’s effect on vein walls. Additionally, constipation (extremely common in pregnancy) causes straining that directly pressurizes rectal veins. What helps: preventing constipation is the primary strategy — 25-30g fiber daily, 8-10 glasses water, and movement. When hemorrhoids are present: witch hazel pads, cool compresses, sitz baths (sitting in a few inches of warm water for 10-15 minutes), and over-the-counter hemorrhoid creams approved for pregnancy (ask your OB or pharmacist). Straining at the toilet makes hemorrhoids worse — try to avoid constipation before it starts rather than managing its consequences.
💦 Increased Sweating — The Thermostat Has Changed
Increased blood volume (now approximately 40-50% above pre-pregnancy levels), metabolic rate elevation, and the baby’s own heat production means your body is generating and managing significantly more heat than it did before pregnancy. Sweating is the primary cooling mechanism, and most women in the second trimester notice they sweat more easily, more profusely, and in situations that previously didn’t cause sweating. Nighttime sweating is common. Wearing breathable, natural-fiber clothing, keeping rooms cool, and staying well hydrated all help. This is normal physiology — not a sign of hormonal imbalance or infection in the absence of other symptoms.
What to Eat at 22 Weeks Pregnant — Calcium for the Surfactant Factory
Surfactant production beginning at Week 22 makes calcium and vitamin D newly critical this week — beyond their role in bone mineralization, both are required for lung tissue development and the type II pneumocyte cell function that produces surfactant.
| Nutrient | Why Critical at Week 22 | Best Sources |
| Calcium | LUNG DEVELOPMENT + surfactant cell function. Also skeleton mineralization continuing, teeth forming. 1000mg/day recommended | Dairy, fortified plant milk, kale, broccoli, almonds, sardines, tofu. Pair with vitamin D for best absorption |
| Vitamin D | Calcium absorption enhancer — without vitamin D, calcium absorption from food is dramatically reduced. Also lung maturation and immune development | Fortified milk, salmon, egg yolks, sunshine (15 min/day safe in pregnancy), vitamin D supplement |
| Iron | Bone marrow continuing full blood cell production — all three lineages. Prevents pregnancy anemia which causes fatigue and affects fetal oxygen supply | Lean beef, dark leafy greens + vitamin C, lentils, fortified cereals |
| Vitamin C | Iron absorption + collagen synthesis (gum health — especially critical for pregnancy gingivitis!). Also lung tissue integrity | Bell peppers, citrus, strawberries, broccoli, kiwi — eat with iron foods |
| Fiber + Water | HEMORRHOIDS + constipation are primary Week 22 digestive issues — fiber and hydration are the prevention strategy | 25-30g fiber + 8-10 glasses water. Prunes, pears, oats, legumes are especially effective |
| Magnesium | Leg cramps (increasingly common), Braxton Hicks frequency management, muscle relaxation, bone density support | Pumpkin seeds, almonds, dark leafy greens, avocado, whole grains, dark chocolate |
Calcium and vitamin D work as a team — calcium provides the raw material; vitamin D is the key that allows the gut to absorb it. Consuming calcium-rich foods without adequate vitamin D results in significantly lower absorption. Most prenatal vitamins contain some vitamin D, but the amounts vary — check yours. Our best prenatal vitamins guide covers which formulas include clinically meaningful amounts of both calcium and vitamin D alongside the other second-trimester priorities.
For Your Partner — Week 22 Meaningful Actions
- Listen for the heartbeat — with just a stethoscope: By Week 22, the fetal heartbeat is audible through a standard stethoscope. Place the stethoscope on the lower abdomen and listen — you may need to try several positions and be patient, but the heartbeat at 120-160 beats per minute is distinctly different from maternal pulse and bowel sounds. This is one of the most accessible, equipment-free moments of connection available at this stage — no Doppler, no medical setting, just a stethoscope and 5 minutes of quiet. If you don’t have a stethoscope, they are inexpensive and widely available. This is worth having for the next 18 weeks.
- Try the flashlight together: Shine a bright flashlight gently against the lower abdomen during a period when the baby is active. Watch for a responding movement — a kick, a roll, a shift. This is one of the earliest forms of direct interaction available to both parents — a small, joyful discovery that the baby is already reacting to the external world. Do it together.
- The viability conversation — have it with information: If the word ‘viability’ has come up in conversation or reading, it’s worth discussing what it actually means. The table in this guide provides survival rate context by week. Understanding the data — that Week 24 is a threshold, not a destination; that outcomes improve dramatically each week from 24-34 — provides a context that converts the word from something alarming into something accurate. Every week from 22 onward is adding to survival and quality-of-life odds in measurable ways.
- Dental appointment — remind and support: Pregnancy gingivitis affects the majority of pregnant women and often goes untreated because of the busy reality of managing a pregnancy. If she hasn’t been to the dentist this trimester, now is the time. Help clear the schedule. The visit is safe, important, and an hour of her day that her gum health will benefit from for the rest of the pregnancy.
- Birth plan research — start together: The hospital bag checklist for mom is one practical starting point, but a birth plan conversation is broader: what are the hospital’s policies on pain management, support people, labor positions, immediate skin-to-skin? Week 22 is the right time to begin the research — not to finalize decisions, but to understand what decisions need to be made before Week 36 when the plan should be in place.
When to Call Your Doctor at 22 Weeks Pregnant
- Heavy vaginal bleeding: Any soaking of a pad or passing of clots — same-day OB contact.
- Severe or persistent abdominal pain: Distinct from round ligament twinges or Braxton Hicks — continuous pain, or pain increasing in intensity, requires evaluation.
- Regular contractions before 37 weeks: Tightenings every 10 minutes or more frequently — OB contact to rule out preterm labor.
- Fluid leaking from vagina: Any persistent trickle or gush of clear fluid — same-day evaluation.
- Significant swelling of face, hands, or one leg: Face/hand: possible preeclampsia — urgent evaluation. One leg: possible DVT — same-day evaluation.
- Shortness of breath at rest or with chest pain: Same-day evaluation.
- Fever above 100.4°F / 38°C: Prompt OB contact.
- No fetal movement established by Week 22-24: If movement hasn’t been felt consistently, mention to OB — especially if no anterior placenta.
Your Week 22 Pregnancy Checklist
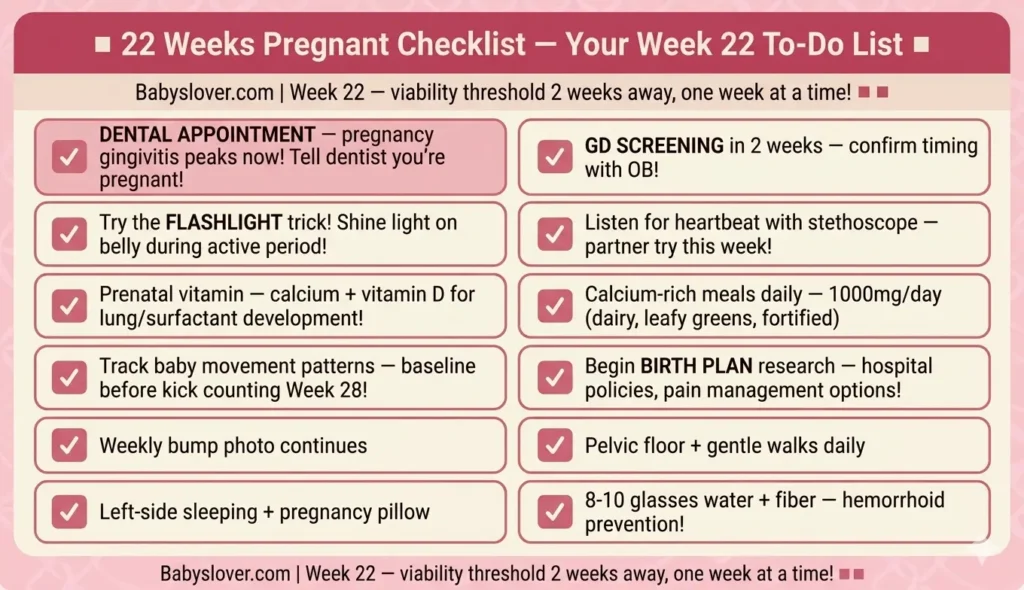
- ☑ 🦷 DENTAL APPOINTMENT — pregnancy gingivitis peaks now! Tell dentist you’re pregnant!
- ☑ 🩺 GD screening in 2 weeks — confirm timing with OB at next visit!
- ☑ 🔦 Try the flashlight trick! Shine light on lower belly during active period!
- ☑ 👂 Listen for heartbeat with a stethoscope — partner try first time!
- ☑ 💊 Prenatal vitamin daily — calcium + vitamin D for lung development!
- ☑ 🥛 Calcium-rich meals daily — 1000mg/day (dairy, leafy greens, fortified foods)
- ☑ 👶 Track baby movement patterns — building a baseline before kick counting at Week 28!
- ☑ 📋 Begin birth plan research — hospital policies, pain management options
- ☑ 📸 Weekly bump photo continues
- ☑ 🏋️ Pelvic floor + gentle walks daily
- ☑ 🌙 Left-side sleeping + pregnancy pillow
- ☑ 💧 8-10 glasses water + 25-30g fiber — hemorrhoid prevention!
Frequently Asked Questions — 22 Weeks Pregnant
How big is my baby at 22 weeks pregnant?
At 22 weeks pregnant, your baby is approximately 28cm long from head to heel (about 11 inches) — the size of an ear of corn — and weighs about 460 grams (around 1 pound). The skin is still thin, reddish, and wrinkled from the visible blood vessels beneath it, and will remain this way until fat deposits build up through the third trimester to smooth it out.
What is surfactant and why does it matter?
Surfactant is a soap-like substance produced by specialized lung cells that coats the air sacs and prevents them from collapsing after each breath. Without adequate surfactant, the effort required to re-inflate collapsed lung sacs with each breath makes sustained breathing impossible. Production begins around Week 22-23 but isn’t sufficient for unassisted breathing until approximately Week 34-36. This is why Week 24 marks the viability threshold — just enough surfactant exists for lungs to be kept open with intensive medical support. Premature babies often receive synthetic surfactant as one of their first treatments in the NICU.
What does viability at 24 weeks mean?
Viability at Week 24 means that a baby born at this gestation may survive with intensive NICU care — not that survival is likely or uncomplicated. Survival rates at 24 weeks are approximately 40-70%, and survivors face significant risks of chronic lung disease, neurological complications, and other long-term health challenges. Outcomes improve dramatically each week from 24 onward. Viability is a medical threshold — the point at which intensive intervention has meaningful chance of success — not a reassurance that birth at this point would be manageable.
What color will my baby’s eyes be?
At Week 22, your baby’s irises have no melanin pigment — which is why almost all babies are born with gray-blue or blue eyes regardless of what their ultimate eye color will be. Eye color develops in the months after birth as light exposure triggers melanin production in the iris. The final eye color typically stabilizes between 6 and 12 months, though some children’s eye color continues changing until age 3. The genetic programming for eye color is established at conception — but it won’t be visible until well after birth.
What is pregnancy gingivitis and how do I treat it?
Pregnancy gingivitis is gum inflammation driven by pregnancy hormones — affecting approximately 60-75% of pregnant women. It presents as swollen, redder-than-usual, tender gums that bleed easily when brushing or flossing. Treatment: soft-bristled toothbrush, gentle circular brushing twice daily, daily flossing (bleeding improves with consistent flossing, not with stopping), alcohol-free antibacterial mouthwash, professional cleaning by a dentist, and staying well hydrated. Tell your dentist you’re pregnant before any procedures. Untreated gum disease in pregnancy has been associated in research with adverse pregnancy outcomes.
Is round ligament pain dangerous?
No — round ligament pain is a normal and harmless pregnancy symptom. It occurs when the round ligaments supporting the uterus are suddenly tensed by rapid movements — rolling over, standing up quickly, sneezing, laughing. The pain is typically sharp, brief, and resolves within seconds to a couple of minutes. Moving more slowly and deliberately when changing position helps prevent it. If pain is severe, persistent for more than a few minutes, or accompanied by other symptoms such as fever, bleeding, or changes in discharge, contact your OB — these features are not characteristic of round ligament pain.
Can I go to the dentist while pregnant?
Yes — routine dental care including professional cleanings is safe and recommended during pregnancy. Untreated dental infections can enter the bloodstream, and pregnancy gingivitis requires professional management for best outcomes. Tell your dentist you’re pregnant and how far along you are; they will avoid unnecessary X-rays and use pregnancy-safe products. Local anesthesia for fillings or procedures is safe in pregnancy. Dental pain should never be left untreated during pregnancy — an untreated dental infection poses more risk than the treatment.
💗 The Emotional Reality of Week 22 — Two Weeks From a Threshold
Knowing that viability week 24 is two weeks from now can land differently for different women.
For some, it’s a marker of progress — a line to cross, a milestone to reach. For others, the number introduces an anxiety that wasn’t there before: what if something happened before Week 24? The honest answer is that between now and Week 24, and indeed all the way to term, the goal is the same: keep growing, keep going, keep building.
The surfactant beginning this week is the clearest evidence of that progress. The grip reflex holding the umbilical cord is another: a functional neuromuscular system testing itself. The heartbeat audible through a stethoscope is another: a heart that has been beating for sixteen weeks, growing stronger and more regular with every day.
Two weeks to viability. Then eighteen more to term. Each one matters.
At Babyslover, we are with you for all of them. 💗
👶 What Happens Next — 23 Weeks Pregnant Preview
23 Weeks Pregnant brings developments that build directly on this week’s foundations:
- 🥭 Large mango — ~29cm, ~500 grams
- VOICE RECOGNITION — baby begins recognizing your voice specifically from other sounds
- SURFACTANT increasing — week-by-week rise toward viability window
- Skin becoming less transparent as fat begins depositing more visibly
- Rapid eye movements in sleep continuing to intensify — REM peak
- Blood vessels in lungs developing the network needed for gas exchange at birth
Keep following our complete pregnancy week by week guide — viability week 24 is one week away from next week’s milestone, and every development between now and then is building toward it. 💗
Week 22: The Corn That Learned to Grip
Being 22 weeks pregnant means carrying a corn-sized person who has grabbed the umbilical cord with a grip strong enough to hold it. Whose lungs have opened the surfactant factory for the first time. Whose eyes are structurally complete but have no color yet — the color is still being written. Who flinches at a flashlight shone through your skin. Whose heartbeat can be heard with a stethoscope, not just a machine.
Two weeks to viability. Eighteen more to term. The corn is growing into a person, week by week.
For everything ahead, our pregnancy tips for first time moms is with you for every week remaining. 💗


1 thought on “22 Weeks Pregnant: Baby Size, Symptoms & Development”